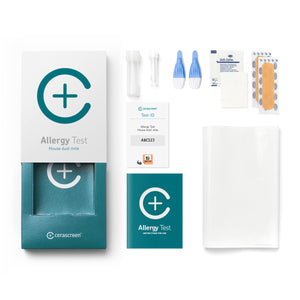
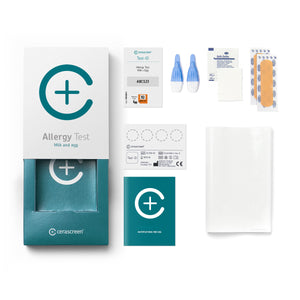
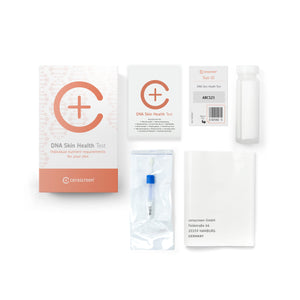
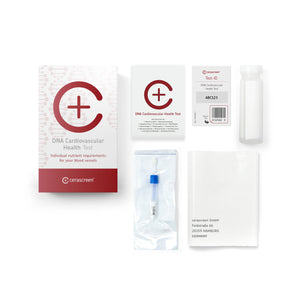
Home health test kits for your health
Choose categoryselftests
health-coaching
all
/blogs/health-portal
/pages/about-us
Get healthy and stay healthy
We don’t always have a good sense of what’s going on in our bodies, nor do we always know what we need in order to get well and stay healthy. The result is that we sometimes suffer from symptoms such as headaches, tiredness, digestive problems, skin rashes or hair loss. A variety of health problems may be lurking behind these symptoms.
Wouldn’t it be great if we had a way to monitor our health on a regular basis? A way to ensure that we are fighting fit? A way to answer questions about whether our blood sugar levels are too high, or if we are deficient in a particular hormone, vitamin or mineral? Well, we have great news: with our home test kits, you will no longer be in the dark when it comes to your health and well-being.
Home health testing: identify problems & take action!
Home test kits have long been more than just questionnaires on the Internet. In order to get well, we need to take a closer look at what is going on inside our bodies, which we can do with cerascreen®’s at-home health test kits. What are your levels of vitamin D and vitamin B12 like? And what about minerals like magnesium, selenium, zinc or iron? Or even proteins and omega-3 fatty acids? Do you suffer from an undiagnosed food allergy or intolerance to histamine, gluten or lactose? Are your cortisol levels or melatonin levels out of balance?
You can get to the bottom of these and many other questions through home health testing. In the comfort of your home, take a blood, breath, saliva, stool or urine sample – depending on the home test kit you’ve chosen – before sending it to our partner laboratory. You’ll then receive a detailed results report that explains what your results mean and which steps you can take to proactively optimise your health.
Test kits from A to Z
So, you may well be asking yourself: What can I measure with home health testing? With cerascreen’s ever-growing range of home test kits, there’s no quick answer to this question. To help you navigate our products, let us tell you about our popular and newest test kits.
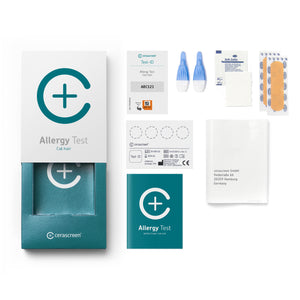
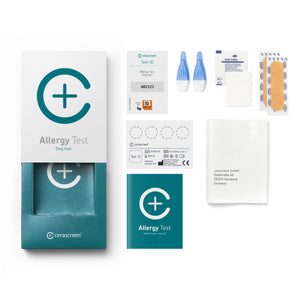
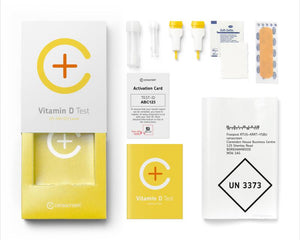
Among our classic bestsellers are the cerascreen® Vitamin D Blood Test and our Vitamin B12 Blood Test – both of which provide critical insights into the levels of these important vitamins in your body. With the Food Intolerance Test and Food Allergy Test, you can test for food intolerances and food allergies. Our Mineral Deficiency Test is a home test kit that checks the concentration of the minerals zinc, magnesium and selenium in your body. But let’s not forget that we can also help you check your cholesterol levels and your long-term blood sugar levels – the latter of which you can use to assess your risk of developing diabetes.
Important recent additions to our collection of at-home health test kits include our Coronavirus (Covid-19) Antibody Test and Covid-19 Vaccine Effectiveness Test, which we consider indispensable in our contribution to fighting the spread of Covid-19 worldwide. The antibody test detects a SARS-CoV-2 infection that has either subsided or been present for a longer period of time. The vaccine effectiveness test will provide you with an indication of whether your vaccination with licensed vaccines has been successful.
Exciting developments at cerascreen mean that you can also test for various allergies and intolerances with our various health test kits – from pollen allergies, food allergies and allergies to house dust and latex. And while we’re on the topic of nutrition, we can help you discover more about your gut health – aka your gut microbiome. Promoting healthy gut bacteria is no small feat, but we can help you take steps to improve your gut health through your diet or through supplements.
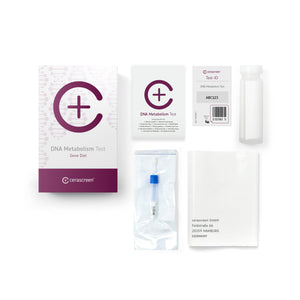
Finally, we are proud to announce our range of DNA home test kits. With these modern genetic self-tests, you can have certain predispositions examined. For example, the DNA Heart Health Test tells you more about your risk of developing cardiovascular problems – so you be proactive about keeping your heart and blood vessels healthy. The DNA Metabolism Test gives you fascinating insights into your performance when it comes to sport and fitness and helps you develop a diet that suits you best.
Leave it to our laboratories
The laboratories that analyse our home test kits are often the same ones that provide analyses for doctors and other medical facilities. In some cases, they are also active in research and involved in the development of new, state-of-the-art home health testing methods. The big difference is that our home health test kits allow you to decide when and where to take a sample – so you can save time spent in waiting rooms or making appointments.
You then send your sample in a return envelope to our medical specialist laboratory. The laboratory analyses your sample, which is then used to write up a detailed and personalised results report that tells you your values, explains the meaning of them and gives you tailor-made recommendations to implement in your everyday life.
Getting well: we’re here to support you
Especially when it comes to a vitamin or nutrient deficiency or food intolerance, the path to optimal health often lies in your own hands. You can give your body what it needs – for example, by altering your diet and/or introducing nutritional supplements.
With an allergy or intolerance, it is often enough just to remove a certain food from your diet or to eat it less often. If you have a confirmed deficiency, dietary supplements should improve your vitamins and minerals levels, melatonin or other sleep improvement supplements will help you catch a better night’s sleep, and probiotics will boost your gut health. If you are not sure where or how to start, don’t hesitate to approach us for help. Nutritional coaching and stress management classes can help you revolutionise your lifestyle and get healthy.